
These facts indicate that it could be important to distinguish atypical pneumonia, especially M. Therefore, the usage of fluoroquinolones as an empirical first choice drug should be limited to only selected patients who have co-morbid illnesses, are of an older age group, have used antibiotics recently, or have severe CAP to prevent an increase in the frequency of quinoline-resistant strains. Furthermore, fluoroquinolone-resistant Haemophilus influenzae has also emerged. pneumoniae has risen markedly and particularly in patients over 60 years of age. In addition, in recent years the incidence of fluoroquinolone-resistant S. Therefore, it is difficult to manage both bacterial and atypical pneumonias by medication with macrolide antibiotics as the first-choice drug. pneumoniae cases show strong resistance to macrolides with minimum inhibitory concentrations greater than or equal to 128 μg/mL. pneumoniae, and especially the high-level of macrolide-resistant S. The etiological matter that most clearly differentiates Asia from Western countries is the frequency of drug-resistant S. However, this test requires paired serum samples with a two to four week interval and provides only a retrospective diagnosis. Serological testing is currently the most common tool for the diagnosis of M. 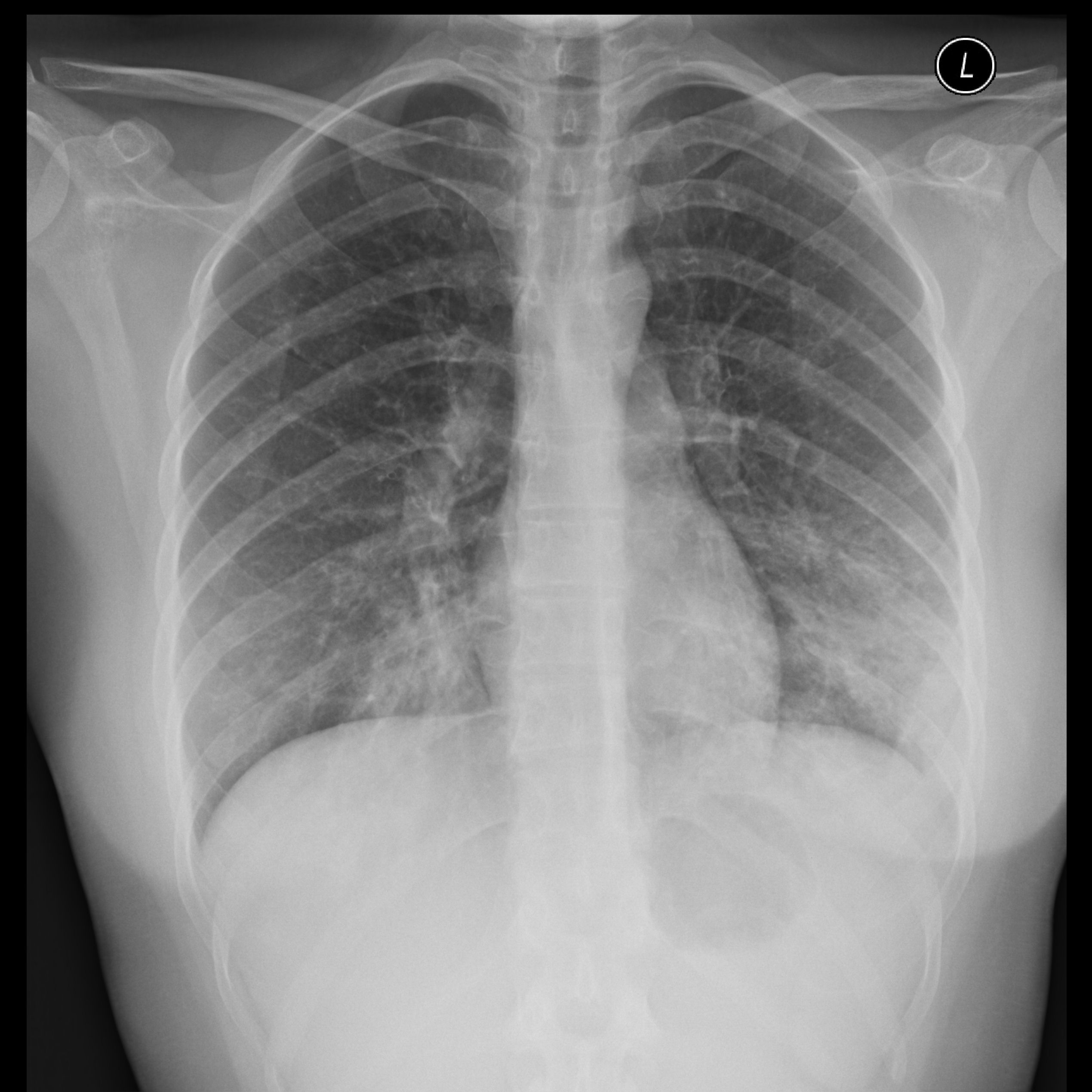
pneumoniae pneumonia is the second leading pathogen of CAP next to Streptococcus pneumoniae. Epidemiological studies in Japan have demonstrated that the incidence of M. 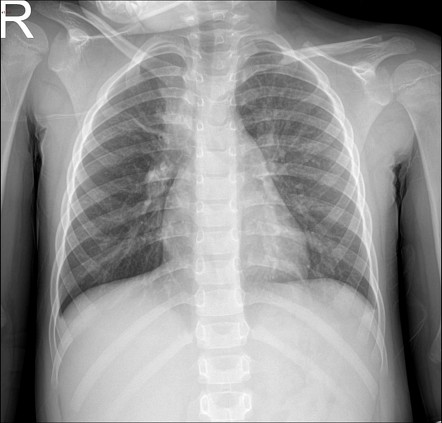
Mycoplasma pneumoniae is one of the most frequent causes of respiratory tract infections, accounting for as many as 10–30% of all cases of CAP. Despite substantial progress in therapeutic options, CAP remains a significant cause of morbidity and death worldwide (the fourth leading cause of death in Japan). Epidemics of Mycoplasma pneumonia occur every 4–8 years in the general population and are more frequent within closed populations (e.g., college dorms, military barracks, and prisons).Community-acquired pneumonia (CAP) is a common infection, which is sometimes fatal. pneumoniae infection in the United States is approximately 1/1,000 persons. Infections occur year-round, but typically in the fall and winter months. It is a common cause of community-acquired pneumonia and is probably responsible for approximately 20–30% of the pneumonias that affect the general population. Mycoplasma is considered an “atypical” bacterium it lacks a cell wall and produces pulmonary infection through extracellular growth and interference with ciliary function. 70.2) and it is therefore referred to as the head cheese sign. The combination of “mixed densities” throughout the lung gives it a geographic appearance similar to a preserved meat product called head cheese or hog’s head cheese ( Fig. 70.1C, 70.1D, 70.1E, 70.1F) acquired on hospital day 4 demonstrates a patchy pattern of variable attenuation characterized by foci of ground glass, consolidation, hypoattenuated lung with reduced perfusion, and intervening areas of normal lung. 70.1B) reveals significant progression of disease. Follow-up AP portable chest exam three days later ( Fig. 70.1A) chest X-ray shows bilateral, perihilar, segmental ground glass and air space consolidations. Two days later, ARDS ensued.Īdmission PA ( Fig. CTPA for pulmonary embolism on hospital day 4 revealed no embolism. Antibiotic therapy was initiated without improvement. 33-year-old man with three- to four-day history of dyspnea, non-productive cough, fevers, and chills admitted to the hospital with presumptive diagnosis of community-acquired pneumonia.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
